Team:SDU-Denmark/Background
From 2009.igem.org

Description of S. aureus
Staphylococcus aureus, also known as golden staph, is the most common cause of staphylococcus infections. It is a gram positive bacterium, that normally can be treated with penicillin. Unfortunately they are becoming more and more resistant to common antibiotics and thereby harder to treat (1).
The nose is regarded as the major site of S. aureus infection and from there the organisms can spread to other parts of the body. About 20% of the human population are long-term carriers of S. aureus. Frequently part of the skin flora is contaminated (2).
Transmission of S. aureus to surgical wound via the skin in patients who are nasal carriers could be an explanation for endogenous infection. Preoperative disinfection is not as effective in the deeper layers of the skin, and S. aureus may thus become a source of infection during surgery (2).
The ability to control staphylococcal infections in the future will depend on many factors, e.g., development of new therapeutic agents, optimization of infection control measures, and introduction of new medical devices with a reduced risk of infection (2).
Pathogenesis
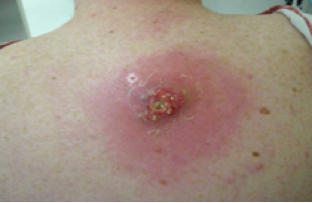
S. aureus is considered a opportunistic pathogen as it can cause infections, while at the same time being part of the normal flora. S. aureus is currently the most common cause of infections in hospitalized patients, with postoperative wound infections being an especially big problem (3).
The success of S. aureus as a pathogen, and its ability to cause such a wide range of infections, are the result of its extensive virulence factors such as toxins (4, 5).
S. aureus infections are plentiful and diverse. The most common infection is of the skin as impertigo, cellulitis or less frequent scalded skin syndrome (5).
If the bacteria enters the bloodstream, a condition known as sepsis, the bacteria can spread to organs with many serious complications, death often being the result (3).
MRSA
Methicillin-resistant Staphylococcus Aureus (MRSA) is defined as a strain of S. aureus that is resistent to beta-lactam antibiotics, which includes common drugs such as penicillins and the cephalosporins (7).
MRSA can cause the same serious infections as other strains of S. aureus, but is especially troublesome, because of it's resistance to the most common antibiotics.
In the United States, invasive (i.e., serious) "MRSA" infections occur in approximately 94,000 persons each year and are associated with approximately 19,000 deaths (8).
Several antibiotics with the ability to kill S. aureus have been made, such as vancomycin and teicoplanin, both drugs that are used to treat MRSA infections today. The absorption of these drugs is very low, for which reason it has to be administrated intravenously. This administration route is not optimal. Moreover new strains has been discovered that are resistant to vancomycin, called VRSA (vancomycin-resistant Staphylococcus aureus) (7).
To be able to treat patients with S. aureus infections in the future, new antibiotics and new methods of treatment most be found.
Biofilm Formation
S. aureus pathogenecity depends on quorum-sensing and biofilm formation. Biofilm is a layer of microbes embedded in an extracellular slime/adhesive, usually polysaccharide material excreted by the cells and attached to a surface (9).
A biofilm facilitates a microenvironment suited for the bacteria. It improves adhesion to the host; it protects the bacteria from hostile environments; and it may confer relative resistance by shielding the bacteria from antibiotics.
S. aureus biofilm formation depends on two quorum-sensing systems, leading to expression of RNAIII that regulates expression of genes involved in pathogenesis. Other staphylococcus strains have developed a RNAIII-inhibiting peptide (RIP) that quenches quorum-sensing, and reduces RNAIII transcription and biofilm formation in S. aureus (10).


Quorum-sensing
Quorum-sensing bacteria produce molecules, termed autoinducers, that function as chemical signal molecules. The concentration of these signals increase as a function of the number of cells in a colony. Using this chemical signaling, the bacteria can adapt to the current situation, and like a multicellular organism synchronize their behavior. The colony of bacteria forms biofilms, that are sessile microbial communities embedded in a self-produced extracellular polymeric matrix, with the advantages described above (12).
The strategy is that bacteria at a low level will express protein factors that promote attachment and colonization, whereas they at lager scale will repress these genes and instead express genes of toxins and proteases, factors that are required for dissemination (13).
In S. aureus the genes involved in quorum-sensing are encoded by the agr-locus (accessory gene regulator) system (12).
Two different promoters P2 and P3 drive the two operons of the arg-locus. The P2 operon codes for a RNAII transcript, while the P3 promoter drives transcription of RNAIII. RNAIII is an important part of the system as it regulates at least 15 genes coding for potential virulence factors (13).
The synthesis of RNAIII is regulated by quorum-sensing molecules. When the autoinducers of the system reach a threshold concentration RNAIII is synthesized. The described autoinducers of RNAIII is RAP (RNAIII activating protein) and the arg- encoded AIPs (autoinducing peptides) (13).
Quorum-quenching using RIP
The ability to disrupt quorum sensing is known as Quorum-quenching.
Quorum-quenching has a great therapeutic potential, since interfering with the bacterial communication can prevent colonization of specific pathogen bacteria that use quorum sensing to coordinate virulence (10).
RNAIII synthesis can be inhibited by different mechanisms. The most potent inhibition is seen by the RNAIII inhibiting peptide (RIP). This peptide is produced by coagulase negative staphylococcus, S. warnerii and S. xylosus. RIP has the sequence YSPXTNF, where X can be a cysteine, a tryptophan, or a modified amino acid.
Native RIP and a synthetic analogue YSPWTHF have been shown effective in inhibiting RNAIII synthesis in vitro and S.aureus infections in vivo (10).
Literature
1. Penicillin; Den store Danske Encyklopædi; 2009.
3. Højby N and Skinhøj P; Klinisk Mikrobiologi og Infektionsmdicin; 3.th edition 1st issue 2008.
5. Staph Infection on medicinenet.com.
6. Image from scmssociety.typepad.com.
7. Wikipedia, MRSA.
8. Klevens et. al; Journal of the American Medical Association 1997; 298 (15);1763-1771
9. Madigan MT and Martinko JM; BROCK BIOLOGY OF MICROORGANISMS, Eleventh edition. 2006. Pearson Prentice Hall. USA
10. Balaban N et al; Regulation of S. aureus pathogenesis via TRAP; JBC Papers in Press. Published on October 16, 2000 as Manuscript M005446200]]
11. Image from Wikipedia.
12. JYarwood JM, Bartels DJ, Volper EM and Greenberg EP. Quorum Sensing in Staphylococcus aureus Biofilms; Department of Microbiology, Roy and Lucille Carver College of Medicine, University of Iowa, Received 21 October 2003/Accepted 1 December 2003
13. Waters CM and Bassler BL; Quorum Sensing: Cell-to-Cell Communication in Bacteria; Department of Molecular Biology, Princeton University, Princeton, New Jersey.
S. aureus
S. aureus is one of the largest causes of hospital infections, each year infecting millions of people around the globe.
S. aureus is normally commensal, but can create bacterial biofilms on implanted medical devices and in post-operational wounds. Biofilm is becoming increasingly hard to treat, as a result of growing resistance to many types of antibiotics.
Brainstorm
Before we decided to work on this project, we had a bunch of other great ideas. You can check out our initial brainstorm here.
Content
Contents |
 "
"


